Modern Treatments
Modern Treatments for Schizophrenia
The brain is the most complex organ of the human body and it therefore follows that it’s disorders are equally complex. Mental disorders such as schizophrenia are very complicated and often cannot be treated successfully by using just one type of medicine. A range of treatments including drugs are available and the key to a successful outcome is to find the right combination of the right drugs and the right talking therapies for the individual patient. Different people will respond differently to different treatments.
Management of the treatment is usually carried out by one of the professionals associated with the case, most often the psychiatrist but the outcome of a successful enduring recovery is more assured if the person with schizophrenia takes some responsibility for their recovery and plays an active role in the management of their treatment. This entails getting to know their condition in a way that the doctor cannot and will result from thorough research in the literature and the internet and many hours of counselling.1
But remember that finding the right treatment regime can be a lengthy process. Finding the right medication at the right dose alongside the most useful talking therapy can take time. Patience is needed along with an understanding that the psychiatrist and the psychiatric nurse do not have all the answers. Different doctors tend to have different approaches to prescribing. Some like to stick with the medicines that they have used successfully in the past whereas others will try out the latest new antipsychotics. Here is what one person with schizophrenia, Bikram said about his doctor’s approach: “” My doctor was really good in that they kept changing the medication to the newest one available. Every time the latest drug came onto the market my doctor would change me on to it. Everyone says that I have been curedby a miracle but it has not yet sunk in on me. How can anyone say that schizophrenia is incurable if we do not yet know completely what causes it?”
One aspect that is hotly debated is when should treatment be started? Some psychiatrists like to take a wait-and-see approach particularly with the first episode but all the evidence points to early intervention being best for the person with schizophrenia and their loved ones. Starting on treatment earlier rather than later ensures a better outcome for the first episode and a reduced chance of further relapses after that.2
Antipsychotic drugs
Why do we use antipsychotics?
Drugs still remain the mainstay of treatment for schizophrenia in the NHS. There are after all a number of antipsychotic drugs that have been in use for many years and have been shown to be very effective in alleviating the positive or psychotic symptoms such as delusions and hallucinations.
The drugs that are prescribed by the doctor to help alleviate the psychotic symptoms are called antipsychotics or neuroleptics. They used to be called major tranquillisers but that term is rarely used now as it is very misleading. These drugs sometimes do have a sedating effect but they are not used specifically for that reason but because of the way they relieve psychotic symptoms.
History of treatments for schizophrenia
Until the middle of the 20th century there were no drugs available for the treatment of schizophrenia and treatment, such as it was, consisted of confining the person in one of the large institutional asylums and administering powerful doses of sedative drugs to restrict their psychotic behaviour. This became known as the chemical cosh.
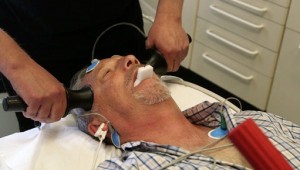
Electro Convulsive therapy involves passing electric current through the brain and remains controversial although its use is now much reduced.
There was also a form of electric shock treatment known as electro-convulsive therapy or ECT which was very controversial and had mixed results. Similarly controversial was shock treatment using large doses of insulin. Brain surgery was also advocated by some as a treatment for schizophrenia.
All of these approaches have largely fallen by the wayside since the introduction of the antipsychotic medicines although ECT is still used in the NHS today in some cases where depression is present and has become deeply entrenched. There is no doubt that ECT got a very bad press over the years but now that the controversy has died down it is recognised that it still has a place in the psychiatrist’s toolkit.12
The first generation of anti-psychotics were developed about sixty years ago and it is thought that they work by influencing the action of a brain hormone called dopamine4, however their precise action is still not fully understood. Chlorpromazine or Largactil was the first antipsychotic and was developed in the 1950s. Originally it was developed as an antihistamine but it was soon found that it was also effective in alleviating the positive symptoms of psychosis.
How effective are antipsychotics?
About 70% of people experiencing psychotic symptoms who take antipsychotics will find their condition improves to some extent: some more so than others5,6. By comparison, this is about the same effectiveness that penicillin has in treating pneumonia.
Antipsychotics do not usually take effect immediately but the benefits will be felt after between three weeks to three months. Different people respond differently to different drugs and finding the right drug at the right dose may take a little time. If a beneficial effect is not seen after a few months then the dose will be increased or the type of medication changed.
The beneficial humanitarian effect of the antipsychotic drugs should not be underestimated. Before the introduction of these drugs in the UK about 70% of people with a diagnosis of schizophrenia were continuously confined in mental hospitals often for years at a time: today it is only about 5% and the average length of stay in hospital is measured in months.3
Antipsychotic drugs can be given as tablets, syrups or as injections including long-lasting injections called depot injections. Depot injections tend to be preferred for people who are not very good at remembering to take tablets.
Types of antipsychotic medicines
Antipsychotic medicines can be divided into two groups. The first generation, which were discovered in the 1950s, known as typicals and the second generation, developed during the 1980s, called the atypicals.
The early, first generation antipsychotics are themselves divided into three groups. All drugs have two names: their generic name and their trade name. You may find the doctor uses either. Below is a list of the most common antipsychotics giving both their generic name and their trade name.
Early antipsychotics: the typicals
Phenothiazine group
Chlorpromazine Largactil
Thioridazine Melleril
Perphenazine Fentazin
Thioxanthine group
Flupenthixol Depixol
Zuclopenthixol Clopixol
Butyrophenone group
Haloperidol Haldol
Droperidol Droleptan
The older typical antipsychotics often have some quite unpleasant side effects including movement disorders known as “extrapyrimidal effects” which include muscle spasms and twitching similar to those seen in people suffering from Parkinson’s disease. These effects can be treated with anti-Parkinsonian drugs such as Procyclidine. For further information on coping with side effects of medication see our information sheet.
Although the first generation of antipsychotics were effective at controlling the positive symptoms of schizophrenia such as hallucinations they had no effect on the negative symptoms such as lethargy.
Second generation antipsychotics: the atypicals
Later on a second generation of antipsychotic drugs was developed. The newer antipsychotics are known as “atypical”. They have fewer unpleasant side effects but are also more expensive. They include:
Risperidone Risperdal
Quetiapine Seroquel
Olanzopine Zyprexa
Amisulpride Solian
Aripripazole Abilify
Sertindole Serdolect
Zotepine Zoleptil
Some of the second generation of antipsychotics are also thought to provide some relief from the negative symptoms.
There is also another antipsychotic which is in a class of its own and deserves a special mention. Clozapine or Clozaril is reserved for people who do not respond to any of the other antipsychotic medicines. It is usually only given if two different antipsychotics have been tried and have failed. It has a number of side effects including an effect on the white blood cell count and consequently regular blood testing is necessary when this drug is prescribed.7
In the NHS treatment guidelines are laid down by NICE, the National Institute for Clinical Excellence, and the current NICE guidelines for treatment of schizophrenia are that the newer atypicals should be chosen in preference to the older typicals for all new cases of schizophrenia and where a person is taking an older typical but is experiencing unpleasant side effects.11
When the symptoms have subsided it will be a good time to think about reducing the dose of the medication to what psychiatrists call a “maintenance dose”. Continuing on this dose will help to reduce the chance of relapse and also help to prevent any residual symptoms that may still be present. It may be necessary to remain on a maintenance dose for a long time sometimes for years after making a substantial recovery.
Other types of medication for people living with schizophrenia
There are two other types of medicine that doctors often prescribe for people with schizophrenia. These are antidepressants and mood stabilisers. Most people with schizophrenia will be offered an antidepressant at some stage in their illness often following the psychotic episode when depression can be a problem.
There are two main groups of antidepressants: the tricyclic antidepressants include amitriptiline, clomipramine, dothiepin, imipramine and lofepramine. The name tricyclic derives from the chemical structure of the drugs.
However it is more common nowadays for one of the more modern SSRI (selective serotonin re-uptake inhibitor) antidepressants to be prescribed. These include citalopram, escitalopram, fluoxetine, fluvoxamine, paroxteine and sertraline. They tend to be safer and easier for the person to tolerate than the tricyclics.
Recently there has been some comment in the media about these SSRI antidepressants leading to agitation and suicidal thoughts in some people. However the jury is still out on that.
Mood stabilisers such as lithium are also sometimes prescribed for people with schizophrenia where mood is a problem.14
Talking therapies and schizophrenia
Antipsychotic medicines are not the only treatments available and nor should they be the only tool in the recovery toolkit. Talking therapies such as counselling and psychotherapy are invaluable in helping people with schizophrenia cope with their symptoms however they cannot treat schizophrenia on their own. Their availability on the NHS is patchy and where they are not available it may be possible to access these services at a centre run by one of the mental health charities such as Mind or Rethink or, in the case of counselling, to find a counsellor who will see you as a private patient.
A weekly session with a good counsellor can be an extremely useful addition to your medication. (Image: Monkey Business Images on Shutterstock)
Counselling
Counselling in particular is to be very highly recommended. A weekly session with a good counsellor can help you cope with the symptoms and also help you cope with the everyday problems that life throws at you. In some areas counselling is available on the NHS and can be accessed through the GP. If there is no local, freely available counselling service then it may be necessary to see a counsellor privately and finance this using the money paid in Disabled Living Allowance. Typically an hour’s session with a counsellor will cost £30 to £50. Counsellors can be found by searching on the internet or by asking at the local library.
Psychotherapy
Coincidentally, at about the time that the chemists were developing the antipsychotic drugs, A.T. Beck, a psychologist in the USA, was working on his ideas for cognitive behavioural therapy or CBT as it is known today. CBT seeks to connect the thoughts that a person is having with the way they feel and how they are acting on their thoughts and feelings. It has been used successfully since then to treat anxiety and depression and has also been found to be helpful with addictions and neuroses like obsessive compulsive disorder.
The role of CBT in schizophrenia is to help the sufferer cope with the delusions and hallucinations without engaging with them. It does not initially seek to challenge the truth or otherwise of the person’s mad ideas. When used in conjunction with medication, CBT has brought welcome relief to many people with schizophrenia.
It is very important to find a good counsellor or therapist. At the very least they should be accredited with the British Association for Counselling and Psychotherapy and it is a good idea to get at least one good reference from a trusted friend before seeing them.

Support groups enable you to meet with other people who are having similar problems. (Image: mangostock on Shutterstock)
Support groups
Support groups can also be extremely useful but their membership may vary from week to week and with it their effectiveness. We have included support groups under the heading of talking therapies but strictly they are in a group of their own as they are often not delivered by a professional practitioner. However many people have had really positive experiences from support groups and have found that the opportunity to discuss their symptoms and their everyday problems with other people who have the same unique experience of the way that psychotic thoughts work has been a valuable part of their recovery.
Family therapy
Studies have shown that the way that a person’s family and friends react to their schizophrenia can greatly affect the pace of their recovery. Families who become very intensely emotional because of their loved one’s behaviour, either hostile or overly concerned, can often obstruct the sufferers pathway to recovery. Psychiatrists call this a high expressed emotion.8 Some NHS areas offer specific family therapy to educate family members about schizophrenia and to help them adopt the most constructive approach in relating to their loved one.

Herbal remedies based on Valerian were prescribed by doctors during the blitz to help with anxiety and insomnia.
Alternative therapies
Unfortunately there is a real lack of hard clinical evidence as to the effectiveness of alternative therapies. Some alternative therapies such as herbal remedies have a track record stretching back centuries. Valerian, for instance, is a longstanding remedy for mental health problems and was widely prescribed for anxiety during the blitz. However some of the newer alternative methods have no such history to support them.
Diet and exercise
There is some evidence that diet has a role to play in maintaining good mental health. Certainly it does seem that one of the first habits to go when a person becomes psychotic is a healthy diet. Every encouragement should be given to people with schizophrenia to have a regular, well balanced diet and to avoid fasting or alternatively junk food and binge eating.

Professor David Horrobin whose pioneering work The Madness of Adam and Eve proposed treating schizophrenia with Omega 3 and 6 supplements.
However some practitioners have gone further than this and suggested that some aspects of diet may be key to good mental health. Professor David Horrobin has undertaken lengthy research into the effect of using Omega 3 and Omega 6 fatty acid supplements to treat positive symptoms and has reported good results even in some patients previously unresponsive to antipsychotics.9 These supplements can be found in cod liver oil and in a purified form as the supplement Omacor. They are also naturally present in oily fish such as salmon, mackerel and sardines. However it should be added that whilst David Horrobin’s early work on this subject showed a great deal of promise, later work carried out by others has not shown as much success.
There has also been some work done on the usefulness of vitamin supplements. There is some evidence that the extrapyrimidal effects of the typical antipsychotics may be alleviated using vitamin E and B6 supplements. There has also been some useful work done in the USA on the role of vitamin and mineral supplements in treating both positive and negative symptoms of schizophrenia itself.10
Frequent exercise is vital. It will not only help to maintain your physical health but it will also help you relax and get a regular sleep pattern. In some areas schemes exist that enable people with long-term health problems to get subsidised membership of a gym. Alternatively you can find out about exercise classes and walking groups on the internet or at the local library.
The importance of having a good diet and plenty of exercise should not be underestimated. People living with schizophrenia also suffer a higher incidence of physical health conditions such as diabetes and heart problems and infectious conditions such as hepatitis and HIV. It is vital that you look after your physical health as well as your mental health.13
Conclusion
Whilst medication remains the mainstay of treatment available on the NHS a better recovery will be assured if it is combined with other types of help especially talking therapies. This help will often not be offered by the NHS practitioners and will need to be sourced locally by the person living with schizophrenia or their family or carers. As soon as the major symptoms have subsided it is a very good thing for the person with schizophrenia to start to play an active role in managing their own recovery.
References
1. Author’s personal experiences.
2. Fuller Torrey E, 2001, Surviving Schizophrenia, Quill, p218.
3. Cutting J and Charlish A, 1995, Schizophrenia, Thorsons, p124.
4. Burton N, 2012, Living with Schizophrenia, Acheron Press, p59.
5. Burton N, 2012, Living with Schizophrenia, Acheron Press, p59.
6. Fuller Torrey E, 2001, Surviving Schizophrenia, Quill, p212.
7. Lintner B, 1996, Living with Schizophrenia, Vermillion, p59.
8. Leff J, 2001, The Unbalanced Mind, Phoenix, p63.
9. Horrobin D, 2002, The Madness of Adam and Eve: How Schizophrenia Shaped Humanity, Corgi
10. Howe G,1986, Schizophrenia a Fresh Approach, David and Charles, p136.
11. Reveley A, 2006, Your Guide to Schizophrenia, Hodder Arnold, p73.
12. Howe G, 1997, Serious Mental illness – A Family Affair, Sheldon Press, p34.
13. Reveley A, 2006, Your Guide to Schizophrenia, Hodder Arnold, p101.
14. Reveley A, 2006, Your Guide to Schizophrenia, Hodder Arnold, p89.







